Orthopedic Surgeon Targets The Complex and Challenging
Orthopedic Surgeon Ed Stolarski Targets “The More Complex and Challenging (Cases), the Better”
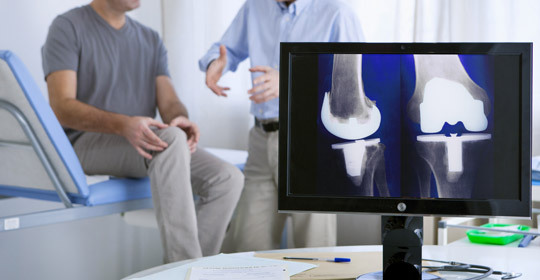
SARASOTA—Board-certified orthopedic surgeon Edward Stolarski, MD, is on track to perform 800 to 1,000 minimally invasive hip and knee replacements this year.
Since relocating from the Cleveland Clinic in Naples, where he helped develop the practice’s total joint replacement program, to the Kennedy-White Orthopaedic Center in Sarasota in 2005, Stolarski has quickly built a solid reputation as one of Florida’s leading orthopedic surgeons. He is an industry leader and developer of new approaches of joint replacement, allowing faster rehabilitation and shorter hospital stays. Among other pioneering moves, Stolarski is training national and international surgeons in the anterior total hip replacements and hip revision techniques.
In 2007, Doctors Hospital of Sarasota named Stolarski Physician of the Year.
“The more complex and challenging the cases are, especially problematic joint replacements, the better,” he said. “It gives me great satisfaction to see the quality of life dramatically improved for my patients after they’ve had joints replaced.”
Stolarski’s case load in patient age ranges from replacing both hips on a 14-year-old girl with juvenile rheumatoid arthritis who had missed 100 days of school and “has gone from being crippled to her mom worrying about her out dating,” he said, to replacing the knee on a very healthy 94-year-old woman who had been confined to a wheelchair and “did just fine.”
The anterior approach for a total hip replacement is a huge benefit for patients, Stolarksi said.
“It’s incredibly minimally invasive with no muscles being cut, hip precautions are greatly reduced, implants are actually put in more accurately, and patients return very quickly to their activities, including yoga, martial arts, as well as high-risk careers such as police work and fire fighters. No special tables are utilized and patient’s leg lengths have been perfect because of how they are positioned. We utilize fluoroscopy in the OR to verify implant positioning and leg lengths. There’s no guesswork.”
Within two weeks of having their joints replaced, most healthy, motivated 40- to 60 year-olds still use some sort of ambulatory aid—crutches or a cane. Within six weeks, they’re playing golf. Within 12 weeks, they’re playing racquet sports. Sometime between six and 12 weeks, they’ll start using weights again.
A large portion of Stolarski’s practice involves revision hip and knee surgery.
“Used to be, people needing a new hip or a new knee were told to wait as long as they could bear it because their implants would only last so long,” he said. “With today’s technology, revisions turn out very well. It’s still a difficult and individual decision as to when a joint replacement should be done for each patient.”
Stolarski, who was an electrical engineer before studying medicine, said his fellowship training in adult reconstruction and the ever-expanding demands for joint replacement led him to focus only on those issues.
“When someone comes in with a problematic hip or knee—it may be as simple as an athlete wanting to get back to playing sports, or as complex as having been bounced around from doctor to doctor with bone loss or infection—the buck stops with me,” he said. “Unless there are other factors, such as medical conditions preventing surgery, most complex revisions can be addressed.”
Even surgeons select Stolarski to perform surgery on them. He replaced a hip in a fellow orthopedic surgeon utilizing the anterior approach and he was working again six days later. He’s also a teacher of surgeons. This November, he’ll be in Henderson, Nevada, conducting the Masters Course for Total Hip Replacements via the Anterior Approach. The attendees are surgeons who are performing this approach, but want to enhance their abilities. “It’s a great educational experience,” he said, “both in the lecture hall as well as the cadaver lab.”
Another new technology Stolarski is exploring and utilizing: patient-specific cutting blocks for total knee patients. By using an MRI of the knee and certain x-rays, a cutting block is made for that individual patient.
“I tell patients it makes me more accurate and reduces blood loss,” he said. “Both of these advantages turn into longer lasting, better functioning knee replacements that are less likely to be painful or need to be redone.”
Stolarski is concerned about one aspect of hip and knee replacements: who will pay for the advanced technology implants and also further research and development.
“I’m worried about it,” he admitted. “For example, I had a 43-year-old male patient who needed a total hip replacement. I wanted to use an implant that was more advanced and cost more than usual. He needed an implant that would last as long as possible. I needed all kinds of OKs before I could do it. My reimbursement doesn’t change with the type of implant, but the implant cost itself is higher. This increased cost is absorbed by the hospital. The problem is that the hospital is reimbursed a set amount, regardless of what I put in a patient. They (the hospitals) are already running on a very thin margin. I realize that hospitals can’t afford to lose money on these procedures, and insurance companies and patients are limited to what they can pay. It’s a very difficult problem that needs to be resolved.”
Getting active people with arthritis back to what they enjoy doing quickly, safely and with minimal disruption in their lives, both short- and long-term, is very rewarding, said Stolarski.
“For the majority of our younger patients, the arthritic joint is the only thing slowing them down, and that’s readily resolved with today’s technology. We focus on techniques and approaches that are minimally invasive and let them lead a normal life.”
SOURCE : by Lynne Jeter http://mana-sara.medicalnewsinc.com/replacing-knees-and-hips-cms-945
Leave a reply